This transcript has been edited for the sake of clarity.
Welcome to Influencing factorComment on your weekly dose on a new medical study. I am dr F. Perry Wilson of the Yale School of Medicine.
I have a love-hate relationship with vitamin D.
A quick search on my blog reveals how I challenged the links between vitamin D and multiple sclerosis, kidney disease, schizophrenia, falls, and educational levels in children.
So it’s no surprise that vitamin D is making a resurgence in the COVID era. I was intrigued when Dr. Anthony Fauci, a sober and responsible voice if there ever was one during this pandemic, reported on his personal use of vitamin D. Vitamin D was also part of the presidential cocktail that Trump received while staying with Walter Reed.
I’ve decided to dig into the data here. But before we do that, let me tell you why I am naturally skeptical of vitamin D studies. There are two main problems:
- Low vitamin D levels have been linked so many things. Vitamin C deficiency causes scurvy – good. But low vitamin D has been linked to everything from Alzheimer’s to whooping cough. It is either the most important vitamin in the world or a substitute for another important thing.
- When we tested all of these fascinating compounds in randomized trials and gave some people vitamin D and a placebo, they almost always showed no effect.
I feel a bit like Charlie Brown with football here. Vitamin D has burned us before. Some examples:
Several observational studies found that people with low vitamin D levels are more likely to develop cancer and cardiovascular disease. These were good studies that adjusted to suitable disruptive factors – the whole business.
Then we received a randomized clinical trial with 26,000 patients. No effect on either result.
Observational studies suggested that low vitamin D levels are linked to the development of diabetes. Then we got a study of 2,400 patients with prediabetes. Vitamin D supplementation had no effect.
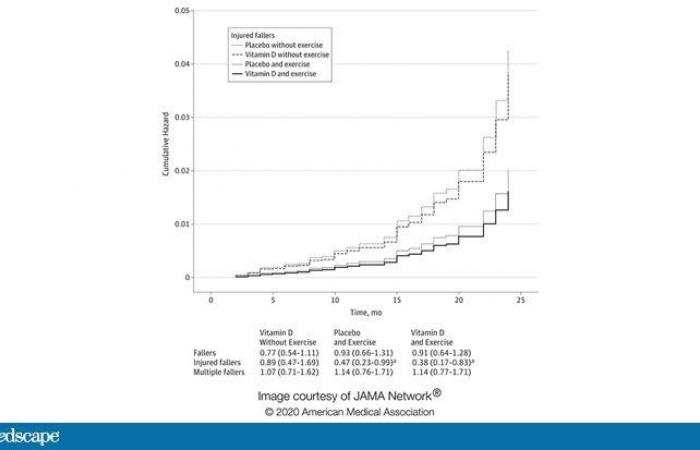
Observational studies have shown that low vitamin D levels are linked to falls. The randomized study found no such effect. (However, practice prevented falls.)
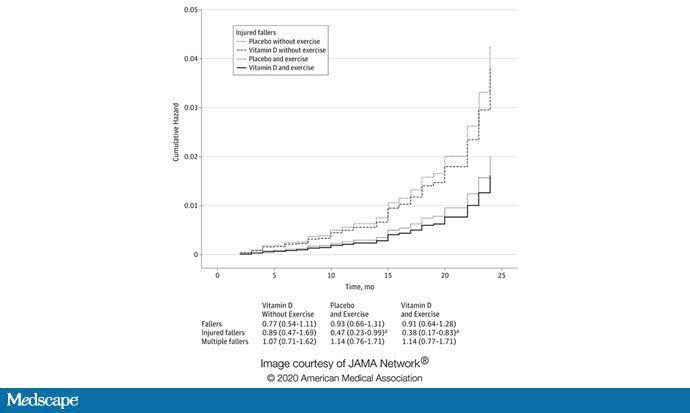
Does Vitamin D Save Lives in General? Not really. In the Women’s Health Initiative study, 36,000 postmenopausal women were randomly assigned to receive vitamin D versus placebo and no survival benefit was found.
I am not saying that vitamin D cannot be used or that it may have limited benefits. Randomized studies are seldom as dramatic as observational data suggests. But I can’t think of any other exposure that has such a wide separation between observational and randomized data.
Why is that?
Because your vitamin D levels are an indicator of the nature of your life and it’s really, really hard to adjust to. Of course, you can ask people how much sun and exercise they’re getting, how varied their diet is, how much money they’re making – but these are pretty blunt tools.
OK. With this in mind, what do we know about vitamin D in COVID?
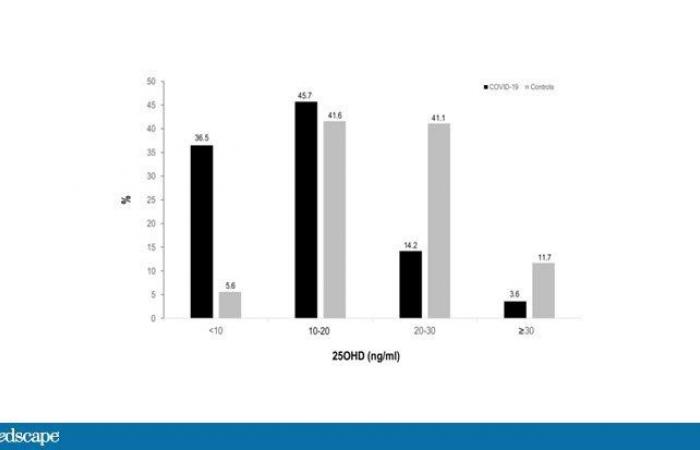
Only this week in the Journal of Clinical Endocrinology & Metabolism, We received this study from Spain which found that out of 216 hospital patients with COVID-19, 80% were vitamin D deficient. Only 40% of the controls were inadequate. Of course, the controls were not hospitalized. Or actually sick.
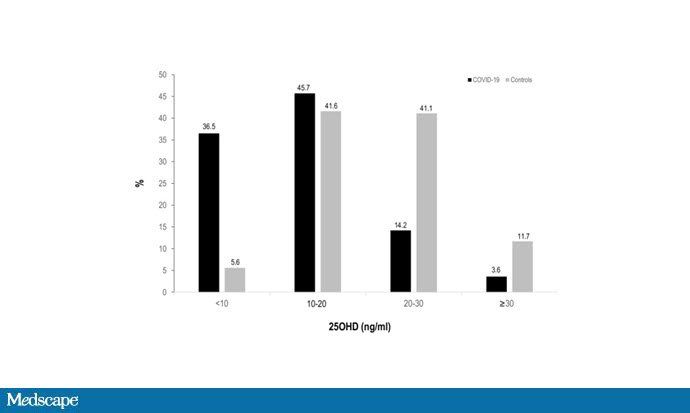
Hernandez JL et al. J Clin Endocrinol Metab. 2020.
But okay, learn better. Back in September, when that record was like 10 years ago, we received this study from Chicago, which showed that out of 489 patients with previous vitamin D tests, those with vitamin D deficiency were 1.77 times higher Were at risk of contracting COVID-19.
That study in PLOS One found that in 235 hospitalized patients, patients with vitamin D levels less than 30 ng / ml had a 20% mortality rate, compared with 9.7% for those with higher levels. I should point out that this article was tagged with an “expression of concern” for some data madness.
Okay, so we did several observational studies – and Anthony Fauci for screaming loudly – and said we should consider vitamin D.
And why not really? That is cheap. It has a pretty harmless side effect profile (though the nephrologist in me worries about kidney stones).
But when it comes to COVID, several factors have been linked to low vitamin D levels also Associated with COVID-19 infection and severity: age, BMI, black race, poverty, comorbidities. It’s just very difficult to adequately account for all of these things statistically.
So I’m shy about vitamin D. I would love a randomized trial. Right now we have one. Two if you squint.
The only randomized study is this one from Spain.
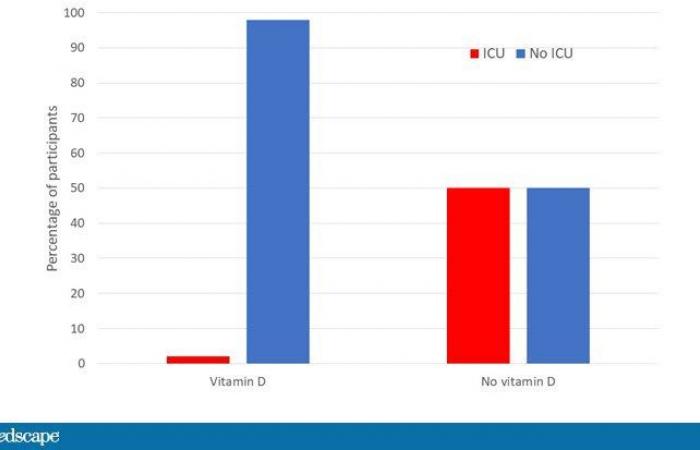
A small study of 76 patients hospitalized with COVID-19 was randomized in a 2: 1 ratio of vitamin D + azithromycin + hydroxychloroquine (don’t start) and azithromycin + hydroxychloroquine alone. Of the 50 people in the vitamin D group, only one went to the intensive care unit. Compare that to 13 of the 26 in the non-vitamin D group.
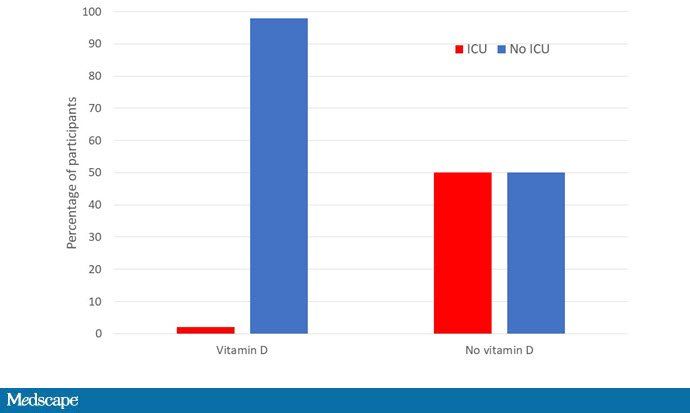
There were no deaths in the vitamin D group and two deaths in the non-vitamin D group. I should note that the non-vitamin D group at baseline was at a slightly higher risk, with more people with diabetes and high blood pressure. But to be honest, it’s the effect size that surprises me here. I mean reducing the risk of ICU admission from 50% to 2%? That’s just an amazing amount. So we are in the space of: Is this a miracle cure or is there a problem with the study that we don’t know about? And miracles are in short supply these days.
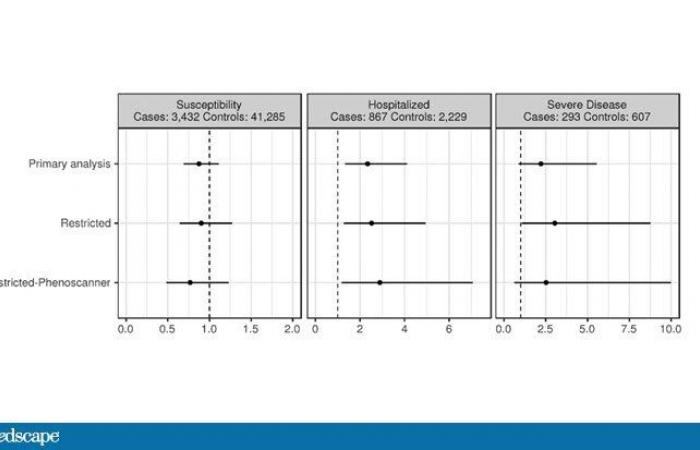
To throw a bit of cold water on this study, we still have it in the preprint, in which Mendelian randomization was used to investigate whether vitamin D could have a causal relationship with the severity of COVID in over 400,000 people.
In this study design, you compare people who are genetically predisposed to lower vitamin D levels with people who do not. That takes lifestyle stuff out of the equation. Interestingly, humans were genetically designed to have low vitamin D levels fewer likely to be hospitalized with COVID-19 or develop a serious illness. Not yet appraised, grain of salt, etc.
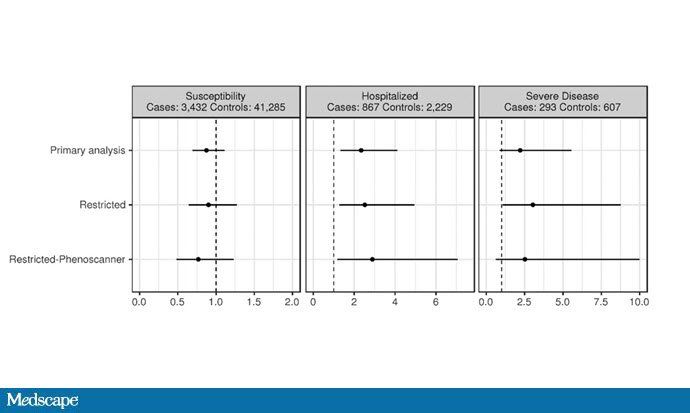
Butler-Laporte G. et al. doi.org/10.1101/2020.09.08.20190975
Bottom line? We know that people with low levels of vitamin D are at greater risk of poor outcomes with COVID-19. We still don’t know if vitamin D supplementation will change that risk. There are some promises here, but the lifestyle vitamin has burned us before. So continue with 400 international precautions.
F. Perry Wilson, MD, MSCE, is Associate Professor of Medicine and Director of the Yale Program in Applied Translational Research. His academic communications work can be found on the Huffington Post, NPR, and here at Medscape. He tweets @methodsmanmd and hosts a repository of his communications work at www.methodsman.com.
These were the details of the news Vitamin D for COVID? We have been burned before for this day. We hope that we have succeeded by giving you the full details and information. To follow all our news, you can subscribe to the alerts system or to one of our different systems to provide you with all that is new.
It is also worth noting that the original news has been published and is available at de24.news and the editorial team at AlKhaleej Today has confirmed it and it has been modified, and it may have been completely transferred or quoted from it and you can read and follow this news from its main source.