The studies – TARGET FFR and DEFINE-FLOW – arrived one after the other in a groundbreaking session at TCT Connect 2020 today.
TARGET FFR found that physiologically controlled PCI did not result in a greater proportion of patients with an optimal FFR ≥ 0.90 in treated vessels; However, the strategy reduced the proportion of patients with a remaining FFR ≤ 0.80. DEFINE-FLOW meanwhile brought the Coronary Flow Reserve (CFR) into the picture as a potential addition to FFR before PCI. Essentially, though complicated, the study found that even a high CFR flow did not negate the importance of a low FFR in determining which cases could be safely deferred.
“We need to pay more attention to the exact physiology we are measuring and what it means,” said Dr. DE LINE Gould (UT Health Science Center, Houston, TX) when speaking to the press yesterday.
Indeed, physiological testing is not just a research tool. The results have clinical consequences. Damien Collison, MB BCh (National Golden Jubilee Hospital, Glasgow, Scotland) presented the TARGET FFR results in TCT’s “Main Arena” and said that below average PCI results could explain why up to 38% of patients 1 year Still reporting angina after treatment.
He noted that the registration data showed high variability in the final FFR, with 21% to 100% of patients achieving scores ≥ 0.90, which was associated with a lower risk of repeated PCI and MACE. “Perhaps more worrisome,” said Collison. Somewhere between 1% and 36% of patients have post-PCI FFRs of 0.80 or less, he noted.
SOUL FFR
Collison and colleagues enrolled 260 patients at their center between March 2018 and 2019 and randomized them after angiographically successful PCI to receive an FFR-guided optimization or a blinded FFR assessment.
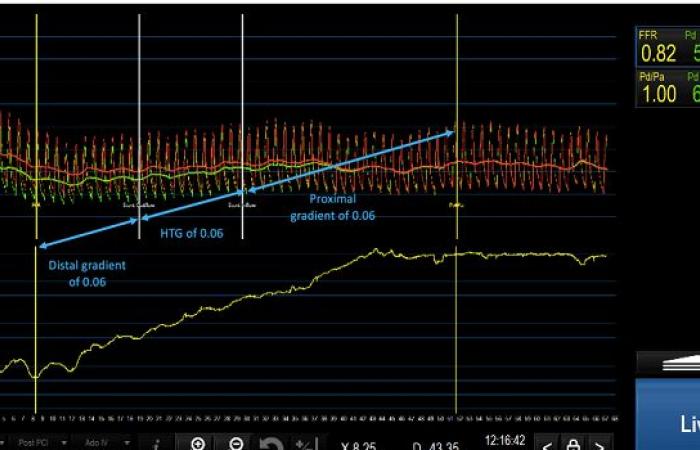
In the guided group, FFR retraction of stent vessels suggested targets for further optimization in 60 of the 131 patients (46%), with operators choosing to perform additional post-dilation and / or stenting in 40 of these subjects (66%). These steps increased the mean FFR after PCI from 0.76 to 0.82, with a larger increase observed during stenting than after dilation, while the CFR increased from 3.0 to 4.0 (P. = 0,02).
“Not unexpectedly, in an analysis in the treated state, additional PCI optimization measures were associated with a longer process duration [plus] higher doses of radiation, contrast, and adenosine, ”noted Collison, adding that there was“ no signal of undue harm ”related to complications.
Overall, the final FFR trended ≥ 0.90 with FFR-driven optimization (38.1% versus 28.1%; P. = 0.099). However, FFR values ≤ 0.80 were significantly less common in FFR-informed treatment after PCI (18.6% versus 29.8%; P. = 0.045). Consistent with previous registration data, the mean FFR values were lower when the target vessel was the LAD versus the left circumflex or right coronary arteries (0.80, 0.92 and 0.91, respectively). P.
The moderator of the session, Dr. Gregg W. Stone (Icahn School of Medicine at Mount Sinai, New York, NY) then asked why the operators decided not to perform further optimization on a third of patients whose FFR suggested improvement. In most cases, Collison replied, there were concerns about the safety of high pressure balloons after stenting, and in some cases the imaging guide may have indicated that additional steps were not required.
Allen Jeremias, MD (St. Francis Hospital, Roslyn, NY), lead author of the DEFINE-PCI In one study, he said he was “a bit shocked” to see that so few patients had optimal FFR after angiographic guidance alone. “It really highlights the importance of doing before and after physiology to guide PCI,” he commented.
DEFINE THE FLOW
In recent years, there has been an increased interest in better understanding microvascular abnormalities, Stone emphasized. “So it is a real pleasure to now look at one of the first real scientific studies to examine the importance of these topics,” he said, introducing DEFINE-FLOW.
The study’s hypothesis was that lesions with abnormal FFR ≤ 0.80 but intact CFR ≥ 2.0 would not have inferior results with medical treatment, “compared to lesions with both FFR and CFR intact,” Dr. Nils Johnson (UT Health Science Center). said in his presentation today.
DEFINE-FLOW researchers participated in 12 sites in six countries and examined 430 patients with 533 stable lesions who were simultaneously FFR and CFR assessed. Only lesions with FFR ≤ 0.80 and CFR
After 2 years, the MACE rates (primary endpoint; death from all causes, MI, and revascularization) differed in the four possible combinations, with the lowest rate in patients with both FFR and CFR negative and the highest in patients with FFR and CFR was positive. Target vessel failure (MI and revascularization) was again lowest in the patients with the best FFR and CFR scores;; It was highest in patients with low FFR but intact CFR.
Biennial Results
| Medical therapy | PCI | |||
| FFR> 0,80 CFR ≥ 2.0 | FFR ≤ 0,80 CFR ≥ 2.0 | FFR> 0,80 CFR | FFR ≤ 0,80 CFR | |
| MORGENSTERN | 5,8% | 10,8% | 12,4% | 14,4% |
| TVF | 3,0% | 9,6% | 6,7% | 6,1% |
Johnson cautioned, however, that there are limitations to consider – not just the observational study, particularly the comparison of treating lesions with positive FFR, but also negative CFR. This “really excludes our ability to make causal statements,” he said. Operators and patients were not blind to the physiological results either.
“DEFINE-FLOW is a hypothesis generating study,” Johnson concluded, adding, “This study has at least taught me personally that we really need to differentiate between the flow to the downstream myocardium and the intracoronary pressure acting against the local plaque. I think it was natural to assume that the myocardium’s ability to increase its flow would really dominate symptoms and clinical events. DEFINE-FLOW suggests that local stress at the stenosis level adds even more to the natural history of atherosclerosis. “
We really need to distinguish between the flow to the downstream myocardium and the intracoronary pressure acting against the local plaque. Nils Johnson
Gould said at the press conference that “this little study is quite important for several, perhaps unclear, reasons.”
Its results undermine the idea that an adequate CFR could overcome an inadequate FFR, allowing for a PCI deferral. However, DEFINE-FLOW results are consistent with results from previous studies of quantitative perfusion in PET imaging, he explained. “The mechanistic explanation could be that the high stress flow (CFR) caused by mild to moderate stenosis or diffuse disease without stenosis causes a drop in coronary pressure. The fluid dynamic equations relating coronary flow pressure predict heterogeneous arterial wall stresses associated with plaque instability, subendocardial ischemia, or both.
“As a result, the high-flow, low-FFR lesion may indicate a less severe stenosis, but still prone to plaque compared to low-flow, low-FFR lesions that may be even more at risk of plaque instability” continued Gould.
A better understanding of what FFR / CFR thresholds are associated with mortality and morbidity could influence study design and “possibly offset the ISCHEMIA and COURAGE studies that are [relied on] precise quantitative severity of the stenosis, ”he said.
Roxana Mehran, MD (Icahn School of Medicine on Mount Sinai) moderated the press conference and said directly that she found the study “a little confusing”. Despite the lack of inferiority, Mehran drew attention in the statistical sense to cases with abnormal FFR ≤ 0.80 but intact CFR ≥ 2.0 as the main area for future studies and asked: “Do we have enough patients? [in DEFINE-FLOW] still to draw very important conclusions because of the permutations of the differential measurements? “
What is clear from large randomized studies – such as MOVE and Fame 2– Is treating low FFR lesions helpful, commented Dr. Chad Rammohan (Sutter Health, Mountainview, CA). It is investigating whether CFR can help determine which patients can safely postpone PCI despite the low FFR. “The process is a little confusing for me as an interventional cardiologist, ”he said, as was the“ double negative ”- that is,“ not inferior ”- in the conclusion.
The general message for now is that FFR should guide decision-making, Rammohan and Mehran agreed, as did Gould. “This study says that primarily at this level you need to trust the FFR [CFR]”Said Gould. “I invented CFR. I would love to see how it works. But I’m a pretty cold blooded scientist. This attempt is very small [and] There are many restrictions. “He said a larger RCT is needed, as well as looking at different CFR thresholds.
For her part, Mehran called for additional studies on CFR, especially in diffuse diseases and in women. “There could also be some gender-specific microvasculature issues that could have an important impact on coronary flow reserve,” she noted.
These were the details of the news FFR Insights before and after PCI: Fresh food for thought for this day. We hope that we have succeeded by giving you the full details and information. To follow all our news, you can subscribe to the alerts system or to one of our different systems to provide you with all that is new.
It is also worth noting that the original news has been published and is available at de24.news and the editorial team at AlKhaleej Today has confirmed it and it has been modified, and it may have been completely transferred or quoted from it and you can read and follow this news from its main source.